Allergy Blood Testing- My Thoughts on Why it is Overused
A recent article in the Wall Street Journal (Is Your Kid Truly Allergic? Tests Add to Food Confusion) recently highlighted the inherent problems with over-calling food allergy in children on the basis of serum IgE testing. I was impressed with the article, and encourage parents of allergic children to read it: http://tinyurl.com/yb5fw5s
This is an issue that most allergists run into on a fairly frequent basis- a parent walks into the office with bloodwork ordered by another physician. Tests returned as "positive" for multiple foods, so for the past 3 months, parents have restricted all these foods (generally there's always something that's a pain in the butt to eliminate, like soy or wheat). Now we have a child who is still as symptomatic as ever, and cranky to boot.
When I tell the parents that their child in all likelihood is not allergic to all of the eliminated foods, the reactions are a mixture of relief and annoyance: "That's great news, but why did we just spend 3 months of our lives wasting a good portion of our paychecks in the gluten/wheat-free aisle at Whole Foods?"
The answer: Because the blood test was ordered without a full understanding of how to interpret the results. The presence of IgE to a specific food does not always translate into clinical allergy.
It is possible to become sensitized to a food, but tolerate it without issue. In these cases, it can actually be counter-productive to eliminate this food, because continuing to eat it in small amounts may be maintaining a state of immune tolerance.
There are multiple nuances in the diagnosis and management of food allergy that simply cannot be delineated by a blood test.
So, why are these blood tests ordered so frequently? The reasons are numerous:
The scenarios in which I use blood allergy testing:
This is an issue that most allergists run into on a fairly frequent basis- a parent walks into the office with bloodwork ordered by another physician. Tests returned as "positive" for multiple foods, so for the past 3 months, parents have restricted all these foods (generally there's always something that's a pain in the butt to eliminate, like soy or wheat). Now we have a child who is still as symptomatic as ever, and cranky to boot.
When I tell the parents that their child in all likelihood is not allergic to all of the eliminated foods, the reactions are a mixture of relief and annoyance: "That's great news, but why did we just spend 3 months of our lives wasting a good portion of our paychecks in the gluten/wheat-free aisle at Whole Foods?"
The answer: Because the blood test was ordered without a full understanding of how to interpret the results. The presence of IgE to a specific food does not always translate into clinical allergy.
It is possible to become sensitized to a food, but tolerate it without issue. In these cases, it can actually be counter-productive to eliminate this food, because continuing to eat it in small amounts may be maintaining a state of immune tolerance.
There are multiple nuances in the diagnosis and management of food allergy that simply cannot be delineated by a blood test.
So, why are these blood tests ordered so frequently? The reasons are numerous:
- Physicians want to help their patients by finding the source of a problem. We're detectives by nature. Because the vast majority of primary care physicians do not have the capability to offer skin testing (more accurate than blood testing) in their offices, blood testing seemingly offers a simple way to provide the same service to their patients.
- There is a misperception among both physicians and the lay public that allergy skin testing is a painful, traumatic process. Physicians and parents feel that they are sparing the child an invasive procedure by choosing a blood test instead. This is inaccurate- allergy skin testing is needleless and bloodless. In the case of a pediatric panel, the testing takes only seconds to apply, and 20 minutes to get results. In contrast, a blood draw requires temporarily restraining the young child while the phlebotomist uses a needle to access a vein (more painful than the superficial scratch from the plastic skin testing device), and then waiting for 1-2 weeks until the test results are delivered to the ordering physician.
- There is the inaccurate assumption that blood testing is more economical that skin testing. This is certainly wrong. The average cost for an individual Phadia Immunocap blood test is $100. In contrast, the average allergy skin test is $10 per item. Some argue that the cost of the blood-based food panels are less than ordering the same tests individually- however, there is generally not value in ordering a panel test which includes foods that the child obviously tolerates- it is a complete waste of resources. In my office, I do not skin test a child to a food that they tolerate without issue. Even when you factor in the cost of the allergist's office visit, skin testing offers a better value, with less wastage of health care resources.
The scenarios in which I use blood allergy testing:
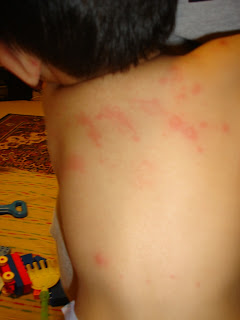
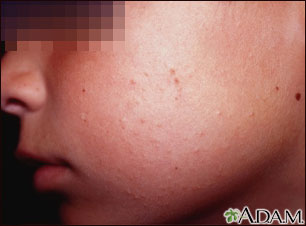
- A child has such extensive eczema that there is not sufficient clear skin on which to apply the test.
- The history of reaction was so immediate and severe (example- life-threatening anaphylaxis from minimal peanut exposure) that it is not prudent to risk the small risk of a systemic reaction from the skin test if the allergy can be confirmed by blood test instead.
- For whatever reason, a child is not able to discontinue antihistamines prior to skin testing.

I've written a lot about allergy blood testing and now write an independent blog for Phadia. You make some very good points, but in all due respect, you may be creating misperceptions about allergy blood tests as well. Your description of a blood test also sounds much harsher than it is. My 6 year old son just had to get an allergy blood test because he had a reaction after getting the flu shot (and happened to eat peanut butter that day) so we weren't sure. He was not restrained in any way, and he didn't mind the teeny prick. He was at ease and left happily. I've heard stories of some children not minding skin prick testing and some being scared out of their wits at the idea of it. It probably depends on how many tests are done and how severe and uncomfortable the reaction is afterwards.
ReplyDeleteAs to the cost, i guess part of the question is, the cost to whom? In my insurance plan, we'd have to pay a $50 co-pay to see an allergist, yet a diagnostic test is free for us. Other plans work differently i know.
Btw, my son had a negative report, meaning he was no allergic to peanuts, and we surmised that it was the small amount of antibiotic in the flu shot that caused the allergic reaction--he had recently had a reaction to zithromax so that's why we made the connection. best, Laurie
Laurie- thanks for your comments! I agree that every child is different, and some children (especially once out of the toddler years) tolerate phlebotomy without any issues whatsoever. However, it has been my experience as a pediatrician (and someone who has been in the position of both drawing blood from a young child and administering skin testing), that the experience for the parent, child, and health care provider is generally easier during skin testing.
ReplyDeleteWhen pediatric skin testing is done appropriately, the number of tests is much lower than it would be for an adult. My environmental panel, for example, includes only 10 small pricks, which are all applied simultaneously (less than 3 seconds to apply the whole shebang).
I must ask why, if your 6 year old son had previously tolerated peanut butter without incident, and there was no reaction within a close time-frame of eating the peanut butter (you mentioned that same day, but not an immediate time-frame), why was peanut allergy even suspected in this case? Without knowing the details of your child's situation, I would venture that the majority of allergists probably would not have recommended either blood or skin testing to peanut in this case, saving you and your child the hassle, and your insurance company the expense.
At the end of the day, the costs that are most important to consider are the costs to the health care system as a whole. Even if you don't get a bill for blood testing, these costs are inevitably rolled into your premiums and those of your neighbors. It may not seem like a big deal in a single case, but when it becomes a trend (as blood-based allergy testing has recently), all the little ripples add up to a very big wave- and larger health care utilization costs for everyone.
Thanks again for your comments- I appreciate the discussion!
Thanks for your thoughts. Re, my son. It was pretty much around the time he was eating peanut butter, and though my pediatrician could have sent us to an allergist for a full assessment, she thought they'd do some preliminary screening test first because of the dangers of peanut allergies and not wanting to lose time (as we were then in peanut-avoidance mode). I've also read that peanut allergies can develop at any time; someone can tolerate them at one point, then become allergic to them later on....
ReplyDeleteI agree with you regarding the total health care cost; Is a physician's visit plus allergy testing less expensive for insurers than the immunocap test?
My 12 month old daughter was given a skin test for an allergy to peanuts and the wheal came back as 14 and the control wheal as 3. The allergist said she was allergic to peanuts and stay away from them. A week later we had a blood test done and her numbers came back as 0. Her doctor again said stay away from the peanuts and we would we test her in 6 to 12 months. So is she allergic or not? And why would the skin test be positive but the blood test be negative? I'm so confused. I'm trying to decide if I should get a second opinion or just wait until her next test.
ReplyDeleteAngel- much of my answer will depend on why your daughter was tested for peanut allergy in the first place. If she experienced a reaction after coming into contact with peanuts, I would trust the skin test and stay away until she can be re-evaluated. Skin testing is known to be more sensitive than the basic blood-based allergen-specific IgE testing. Interestingly, in the absence of clinical symptoms, my advice might be different, because many children who tolerate peanuts quite well have developed positive skin test reactions due to cross reactivity with birch pollen. However, since I am not familiar with your child's history, I cannot offer any specific recommendations for you. If you are interested in obtaining a second opinion, you can find Board-certified allergists through the American Academy of Allergy, Asthma & Immunology (http://www.aaaai.org)or the American College of Allergy, Asthma & Immunology (http://www.acaai.org).
ReplyDeleteMy son is SUPER NEEDLE PHOBIC. We did not know what the skin testing would involve and after our little guy had shaken the nurses hand and gotten a firm promise from her (yes, he's two and a half) and a firm promise from us (well, actually ten or twelve such firm promises), he had to be restrained and cried terribly during his skin testing which to him felt like needles pricking him. Are there any books or websites out there about helping kids prepare for skin testing? And by the way, when did all the kids start having so many allergies, seems like a totally new trend to me. My son is adopted and allergies run three generations deep in his bio-family but nearly non-existent in my family. And I can't say I ever really knew anyone with these severe of allergies growing up.
ReplyDeleteSakina, I found your blog post insightful and valuable. Thank you.
ReplyDeleteDo you know if higher incidence of allergies correlate with early weaning from the breast? Are the occurrences smaller the longer a child is breastfed?
Next, my 3 year old has a mild hearing loss due to fluids in his middle ears. He hasn't had recurring ear infections. We are now thinking it could be a dairy intolerance causing inflammation in his eustachian tubes, preventing the fluids from draining. Right now we are eliminating dairy from our diets to see if his speech improves. It's only been a week, so nothing noticeable yet. We are probably going to get him allergy-tested next week. We don't want to put tubes in his ears if it's an allergy issue. Have you ever dealt with a similar situation?
Thanks for this. I really like what you've posted here and wish you the best of luck with this blog and thanks for sharing. Allergy Testing
ReplyDelete